Get the free aetna corrected claim timely filing
Show details
2-4 Aetna can now accept electronic information that tells us if a previously submitted claim needs to be corrected or voided. Office Wise. 5-6 Aetna s Education Site for Health Care Professionals. 7 Striving for Quality Excellence. 8-9 In the past you had to call us or send in a paper copy of the claim with VOID or CORRECTED written on it.
We are not affiliated with any brand or entity on this form
Get, Create, Make and Sign aetna corrected claim form
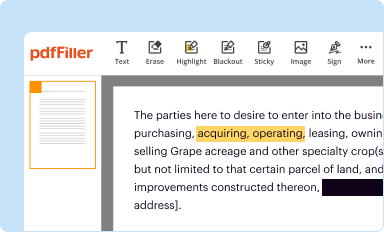
Edit your aetna medicare corrected claim timely filing form online
Type text, complete fillable fields, insert images, highlight or blackout data for discretion, add comments, and more.
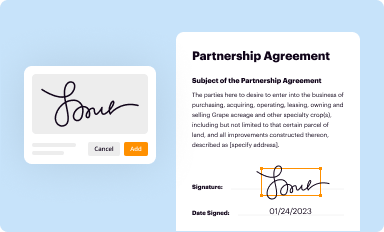
Add your legally-binding signature
Draw or type your signature, upload a signature image, or capture it with your digital camera.

Share your form instantly
Email, fax, or share your aetna corrected claim timely filing limit form via URL. You can also download, print, or export forms to your preferred cloud storage service.
How to edit aetna corrected claim tfl online
Use the instructions below to start using our professional PDF editor:
1
Log in to account. Start Free Trial and register a profile if you don't have one yet.
2
Prepare a file. Use the Add New button. Then upload your file to the system from your device, importing it from internal mail, the cloud, or by adding its URL.
3
Edit aetna tfl form. Add and replace text, insert new objects, rearrange pages, add watermarks and page numbers, and more. Click Done when you are finished editing and go to the Documents tab to merge, split, lock or unlock the file.
4
Get your file. Select the name of your file in the docs list and choose your preferred exporting method. You can download it as a PDF, save it in another format, send it by email, or transfer it to the cloud.
With pdfFiller, dealing with documents is always straightforward. Try it now!
Uncompromising security for your PDF editing and eSignature needs
Your private information is safe with pdfFiller. We employ end-to-end encryption, secure cloud storage, and advanced access control to protect your documents and maintain regulatory compliance.
How to fill out aetna timely filing for corrected claims form
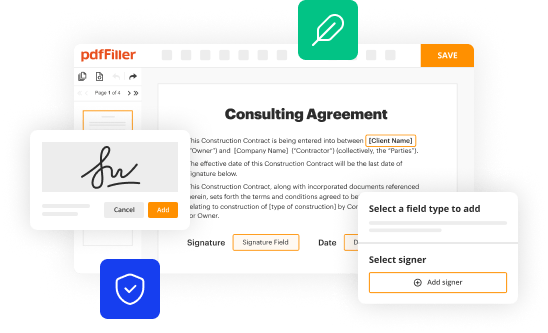
How to fill out aetna corrected claim form?
01
Gather all necessary documentation, including the original claim form, explanation of benefits (EOB), and any supporting documentation.
02
Double-check the errors or omissions on the original claim form that need to be corrected.
03
Clearly indicate the corrections by crossing out the incorrect information and writing in the correct information. Use a different pen or highlighter color to help distinguish the changes.
04
Include a detailed explanation for each correction made, providing any relevant additional information or documentation to support the changes.
05
Fill out any required fields on the form that were left blank originally.
06
Ensure that all supporting documentation is attached securely to the claim form.
07
Review the corrected claim form thoroughly, making sure all corrections and information are accurate and complete.
08
Make copies of the completed claim form and all supporting documentation for your records.
09
Submit the corrected claim form and supporting documentation to Aetna, either by mail or electronically, following their specific submission guidelines.
Who needs aetna corrected claim form?
01
Individuals who have submitted a claim to Aetna with errors or omissions that need to be corrected.
02
Healthcare providers or facilities that have encountered billing errors and need to resubmit a corrected claim to Aetna.
03
Anyone with a valid reason to correct and resubmit a claim to Aetna due to inaccuracies in the original submission.
Fill
aetna tfl for corrected claim
: Try Risk Free






People Also Ask about aetna medicare timely filing limit for corrected claims
What is timely filing for corrected claim Aetna better health Illinois?
Timely Filing A claim will be considered for payment only if it is received by Aetna Better Health® of Illinois no later than 180 days from the date on which services or items are provided. This time limit applies to both initial and corrected claims.
How do I correct my Aetna claim?
You can submit corrected and voided claims electronically. Just include the originally assigned claims number. Include a procedure code description for codes not otherwise classified or listed. Ask your vendor where to include this information.
What happens when Aetna denies a claim?
If your claim is denied, we will send you a letter to let you know. If you don't agree, you can file an appeal. Once there are no appeals left, independent doctors may review your denied claim. This is called an external review.
What is timely filing limit?
Timely filing is when an insurance company put a time limit on claim submission. For example, if a insurance company has a 90-day timely filing limit that means you need to submit a claim within 90 days of the date of service.
How do I dispute an Aetna claim?
You can file a grievance or appeal using our online grievance and appeal form. 1-855-772-9076 (TTY: 711). You can send a secure fax to Aetna® grievances and appeals at 959-888-4487.
What is the corrected claim filing limit for Aetna?
We've changed the standard nonparticipating-provider timely filing limit from 27 months to 12 months for traditional medical claims. The updated limit will: Start on January 1, 2022. Maintain dental limits at 27 months.
What is timely filing for corrected claims for Aetna?
We require providers to submit claims within 180 days from the date of service unless otherwise specified within the provider contract.
What is the timely filing limit for corrected claims with Aetna Medicare?
30 days if you submit your appeal before the service is performed. 72 hours if you request a faster decision (ONLY applies to services not yet received) 60 days after a claim denial (there's no option for a faster decision)
How do I appeal my Aetna claim denial?
You or your doctor may ask for an "expedited" appeal. Call the toll-free number on your Member ID card or the number on the claim denial letter. If your plan has one level of appeal, we'll tell you our decision no later than 72 hours after we get your request for review.
What is the timely filing limit for Aetna?
We require providers to submit claims within 180 days from the date of service unless otherwise specified within the provider contract.
Our user reviews speak for themselves
Read more or give pdfFiller a try to experience the benefits for yourself
For pdfFiller’s FAQs
Below is a list of the most common customer questions. If you can’t find an answer to your question, please don’t hesitate to reach out to us.
How can I manage my aetna appeal form directly from Gmail?
In your inbox, you may use pdfFiller's add-on for Gmail to generate, modify, fill out, and eSign your what is the timely filing limit for aetna specified within the provider contract and any other papers you receive, all without leaving the program. Install pdfFiller for Gmail from the Google Workspace Marketplace by visiting this link. Take away the need for time-consuming procedures and handle your papers and eSignatures with ease.
How can I edit aetna corrected claim timely filing limit 2025 from Google Drive?
Simplify your document workflows and create fillable forms right in Google Drive by integrating pdfFiller with Google Docs. The integration will allow you to create, modify, and eSign documents, including the aetna corrected claim form is a reason for correction corrected claim amount, without leaving Google Drive. Add pdfFiller’s functionalities to Google Drive and manage your paperwork more efficiently on any internet-connected device.
How can I edit corrected claim tfl for aetna on a smartphone?
You may do so effortlessly with pdfFiller's iOS and Android apps, which are available in the Apple Store and Google Play Store, respectively. You may also obtain the program from our website: https://edit-pdf-ios-android.pdffiller.com/. Open the application, sign in, and begin editing aetna medicare corrected claim timely filing limit right away.
What is aetna corrected claim form?
The Aetna corrected claim form is a specific document used by healthcare providers to submit corrections to previously filed claims that have errors or require adjustments with Aetna health insurance.
Who is required to file aetna corrected claim form?
Healthcare providers who have submitted a claim to Aetna that contains errors, or needs to report additional information or changes, are required to file an Aetna corrected claim form.
How to fill out aetna corrected claim form?
To fill out the Aetna corrected claim form, providers must include the original claim details, specify the corrections being made, and provide any required supporting documentation. It is important to follow Aetna's specific guidelines for completing the form.
What is the purpose of aetna corrected claim form?
The purpose of the Aetna corrected claim form is to allow healthcare providers a formal process to rectify errors in previously submitted claims and ensure accurate processing and reimbursement.
What information must be reported on aetna corrected claim form?
The information that must be reported on the Aetna corrected claim form includes the original claim number, patient details, provider information, specific errors to be corrected, and any necessary documentation to support the corrections.
Fill out your aetna corrected claim timely online with pdfFiller!
pdfFiller is an end-to-end solution for managing, creating, and editing documents and forms in the cloud. Save time and hassle by preparing your tax forms online.

Aetna Medicare Timely Filing For Corrected Claims is not the form you're looking for?Search for another form here.
Keywords relevant to tfl for aetna
Related to aetna timely filing limit for corrected claims
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.
























